Challenge
Oral health disparities are profound among low-income, minority and rural children due to poor access and the inability to afford care.
Oral health disparities are profound among low-income, minority and rural children due to poor access and the inability to afford care.
The Duke Endowment is supporting the expansion of school-based oral health programs and investing in advocacy and policy efforts to incentivize the proliferation of those programs in the Carolinas.
By the fall of 2021, 28 school-based oral health programs were providing dental care to 343 schools throughout the Carolinas.
A full understanding of root causes is necessary to address system flaws, better identify solutions and make meaningful change. Addressing these systemic issues takes time, investment, relationship building and collaboration.
Oral health disparities are profound due to poor access and the inability to afford care. Low-income, minority and rural children suffer disproportionally from problems related to oral health. Tooth decay is the single most common chronic childhood disease, and dental disease is responsible for a collective 51 million hours of school missed each year. The rate of tooth decay among Hispanic and African American children ages 2 to 8 is twice that of white children; preschool-age Native Americans experience four times as many cases of untreated tooth decay.
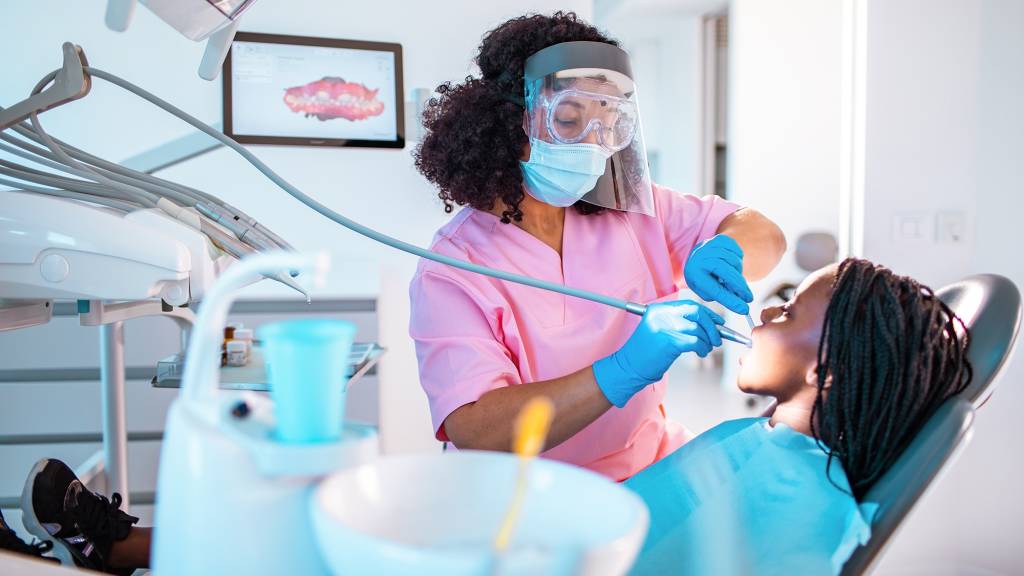
School-based oral health prevention programs are an effective way to mitigate dental disease in children. Research has shown that school-based programs can reduce dental disease by 50 percent, remove barriers to care and decrease missed education time. They also ensure that children receive recommended preventative care such as sealants, which are 80 percent effective in preventing dental disease.
To reduce oral health disparities in children, The Duke Endowment is helping school-based oral health programs expand to ensure that vulnerable children have access to essential dental care. We are also investing in advocacy and policy efforts that will incentivize the proliferation of sustainable school-based oral health programs throughout the Carolinas.
While school-based programs are effective, they haven’t been widely replicated due to the complexities of integrating them within the education system and the challenges of establishing a sustainable business model. To better understand these hurdles, The Duke Endowment funded a case study of eight programs to evaluate their comparative effectiveness and viability for replication. These pilots taught us that while it is possible to develop a sustainable and scalable model for providing dental services within schools, new programs would need extensive technical assistance and capacity building before implementation.
In 2018, we partnered with the Blue Cross and Blue Shield foundations in both Carolinas to launch the school-based Oral Health Expansion Initiative. We used the Medical University of South Carolina’s College of Dental Medicine and East Carolina University School of Dental Medicine for technical assistance and ongoing consulting with grantees.
The state implementation teams developed 15 web-based didactic training modules and consolidated various templates and resources on an online portal. Each grantee is required to participate in a nine-month readiness phase with the state implementation teams to ensure that they have an advanced clinical care plan, a viable business plan, and adequate financial and clinical data reporting capabilities. Once participants complete the readiness phase, they are eligible to apply to the Endowment for a two-year implementation grant.

In November 2018, the Endowment funded the first cohort of 10 grantees to work with our technical assistance teams. The first group secured 102 Head Start centers, elementary, middle and high schools as partners for the 2019 – 2020 academic year. They began services in September 2019, and during the seven months before schools were closed in March 2020 due to the pandemic, they served 9,700 children with over 18,000 treatment services. This significantly exceeded our projections.
In 2019, we selected 12 new grantees for the second readiness and planning cohort. Eleven of the 12 successfully completed the requirements and are prepared for implementation. In the fall of 2020, we selected 10 grantees for the third cohort, for a total of 31 grantees in this initiative. Blue Cross and Blue Shield of North Carolina Foundation and BlueCross BlueShield of South Carolina Foundation have partnered with the Endowment and contributed $1.4 million to fund the readiness and planning phases for the second and third cohorts. As of 2022, 28 organizations have successfully implemented or have expanded school-based oral health programs and are providing services in hundreds of high risk schools throughout North Carolina and South Carolina.
To strengthen our school-based Oral Health Expansion Initiative and to ensure that this program could be scaled and sustained, we recognized that policy and reimbursement changes were critical. Our investments in this area have increased our understanding of oral health disparities and opportunities to improve the delivery system. We have learned that advocacy and policy work takes time and that success depends on building relationships and trust.
Our first significant policy win was on February 16, 2020, when a rule change was passed to expand dental hygienists’ scope of practice regulations, which increased the efficiency and viability of our program in schools. The change allows dental hygienists to practice to the full extent of their licensure by providing preventive services such as sealants and fluoride treatments without a dentist’s prior exam. This milestone, supported by the North Carolina Oral Health Collaborative and the North Carolina Dental Society, is one that we had aspired to for nearly a decade. The victory ensures that our school-based programs are more sustainable, and it has established the North Carolina Oral Health Collaborative as a credible resource for policy.
Years of groundwork have paved the way to an environment that is more open to change. This, coupled with the pandemic, is providing an opportunity to make lasting advances in the field. Two examples include:

This initiative has taught us a tremendous amount about systems work. We have learned that even good programs are not enough to tackle complex problems and make lasting change. For meaningful improvements, system flaws need to be addressed, which generally requires a full understanding of root causes. Understanding the “why” has helped us better identify solutions. We’ve also learned that addressing systemic issues is difficult and takes significant time, investments, relationship building and collaboration to advance the work.
October 11, 2018 | Dr Elizabeth Pilcher and Dr. Michelle Ziegler